Dengue fever
| Dengue fever | |
|---|---|
| Classification and external resources | |
 The typical rash seen in dengue fever | |
| ICD-10 | A90. |
| ICD-9 | 061 |
| DiseasesDB | 3564 |
| MedlinePlus | 001374 |
| eMedicine | med/528 |
| MeSH | C02.782.417.214 |
Dengue fever (pronounced "DEN-gi") is a tropical infectious disease caused by the dengue virus. People get the dengue virus from mosquitoes. Dengue fever is also called break-bone fever, because it can cause so much pain that people feel like their bones are breaking.
Most people with dengue fever can get better just by drinking enough water. However, a small number of people get dengue hemorrhagic fever or dengue shock syndrome. These are medical emergencies and can kill a person if they do not get medical treatment.
There is no vaccine that can keep people from getting the dengue virus. There is also no treatment to cure dengue fever. Doctors can only provide "supportive care," which means they can only treat dengue's symptoms.
Since the 1960s, more people have been getting dengue fever. Since World War II, dengue has become a problem around the world. It is common in more than 110 countries. Every year, between 50 million and 100 million people get dengue fever. Climate change means that there are more mosquitoes. In Brazil it is expected that there will be at least twice as many cases in 2024 than in 2023.[1]
Signs and symptoms[change | change source]
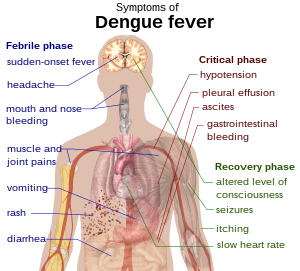
80% of people who get the dengue virus have no symptoms, or have only mild symptoms (like a basic fever).[2][3][4] About 5% of infected people get much sicker. A small number of these people have symptoms that could kill them.[2][4]
After a person gets the dengue virus from a mosquito, it takes between 3 and 14 days for them to get sick. (This is called the virus's incubation period.) [5]
Often, when children have dengue fever, their symptoms are the same as gastroenteritis (stomach flu), like vomiting and diarrhea, or the common cold.[6] Children are more likely to have bad complications from dengue fever.[7]
Dengue fever happens in three stages: febrile, critical, and recovery.[8]
The febrile stage[change | change source]
In the febrile stage, people with dengue usually have a high fever. ("Febrile" means that a person has a fever.) The fever is often over 40 degrees Celsius (104 degrees Fahrenheit). Sometimes the fever gets better, and then comes back.[9][10]
During the febrile stage, people may also have:[7][11][12]
- Pain all over their bodies
- A headache
- A rash (this happens in 50% to 80% of people who get sick from dengue)
- Petechiae (small red spots on the skin). These are caused by capillaries (which carry blood) breaking. This makes the blood leak out and show up under the skin.
- Small amounts of bleeding from the mucous membranes in the mouth and nose
The febrile stage usually lasts 2 to 7 days.[8][11] This stage ends when a person's high fever is gone.
The critical stage[change | change source]
In about 5% of people with dengue fever, the disease goes into a critical stage next.[7] ("Critical" means "very dangerous.") The critical phase usually lasts 1 to 2 days.[8] Plasma (the liquid part of blood) leaks out of the body's small blood vessels. The plasma can build up in the chest and abdomen. This is a serious problem.
Plasma carries blood cells, glucose (sugar), electrolytes (salts), and many other important things to the whole body. Every part of the body needs these things to survive. If too much plasma leaks out of the blood vessels, there will not be enough left to carry these things to the body's most important organs.[8] Without these things, the organs cannot work normally. This is called dengue shock syndrome. Plasma also carries platelets, which help the blood clot (they help stop bleeding). If a person does not have enough platelets, they can have dangerous bleeding. With dengue fever, this bleeding usually happens in the gastrointestinal tract.[7][8] When a person has bleeding, leaking plasma, and not enough platelets, they have dengue hemorrhagic fever. ("Hemorrhage" means "dangerous bleeding.")
The recovery stage[change | change source]
The recovery stage is when the patient's body is overcoming the disease process. In this stage, the plasma that leaked out of the blood vessels is taken back up into the bloodstream.[8] This stage usually lasts 2 to 3 days.[7] During this stage, people with dengue often feel much better. However, they can have very bad itching and a slow heart rate.[7][8]
Serious problems can also happen during the recovery stage. If a person's body takes too much fluid back up into the bloodstream, this can cause "fluid overload." This can cause fluid to build up in the lungs, which causes breathing problems. Fluid overload can also cause seizures or an altered mental status (changes in a person's thinking and behavior).[7]
Complications[change | change source]
Dengue can affect other systems in the body.[8] It can cause:
- Altered mental status: This happens in 0.5% to 6% of people with very bad dengue fever. It can happen when the dengue virus causes an infection in the brain. It can also happen when important organs, like the liver, are not working correctly because of dengue.[6][10]
- Neurological disorders: These are problems with the brain and the nerves, like Guillain–Barré syndrome [6] and Post-dengue acute disseminated encephalomyelitis.[13]
- Infection of the heart, or sudden liver failure (these are very uncommon).[7][8]
Cause[change | change source]
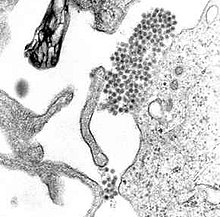
Dengue fever is caused by the dengue virus. In the scientific system that classifies viruses, the dengue virus is part of the family Flaviviridae and the genus Flavivirus. Other viruses that belong to the same family and can make humans sick include yellow fever virus, West Nile virus, Zika virus, Japanese encephalitis virus, and tick-borne encephalitis virus.[10] Most of these viruses are spread by mosquitoes or ticks.[10]

Dengue virus is spread mostly by mosquitoes from the Aedes genus, especially the Aedes aegypti species of mosquito.[3] Aides aegypti is the most likely type of mosquito to spread dengue, because it likes to live close to humans and feed off of people instead of animals.[14] A person can get the dengue virus from just one mosquito bite.[15]
Sometimes, mosquitoes can also get dengue from humans. If a female mosquito bites someone with dengue, the mosquito may get the dengue virus from the person's blood. After about 8 to 10 days, the virus spreads to the mosquito's salivary glands, which make saliva (or "spit"). Now the mosquito will make saliva that is infected with the dengue virus. When the mosquito bites a human, its infected saliva goes into the human and can give that person dengue.
A person can also get the dengue virus if they get a blood transfusion or organ donation from someone who has the virus.[16][17] In some countries where dengue is common, like Singapore, between 1.6 and 6 blood transfusions out of every 10,000 spread dengue.[18]
The dengue virus can also be spread from a mother to her fetus during pregnancy, or when the child is born.[19] This is called vertical transmission.
Dengue is usually not spread in any other ways.[11]
Dengue virus in the human body[change | change source]
Once a person gets the dengue virus from a mosquito, the virus attaches to and enters the person's white blood cells. (The white blood cells are part of the immune system, which defends the body by fighting off threats, like infections.) As the white blood cells move around the body, the virus makes copies of itself. The white blood cells react by making many special proteins, like interferon, which tell the immune system to work harder because there is a threat in the body. These proteins cause the fever, flu-like symptoms, and severe pains that happen with dengue.
If a person has a bad infection, the virus makes copies of itself much more quickly inside the body. Because there is a lot more of the virus, it can affect many more organs (like the liver and the bone marrow). The virus can stop the bone marrow from making platelets normally. This makes very bad bleeding much more likely to happen.[20]
Risk factors[change | change source]
Babies and young children with dengue are more likely than adults to become very sick. Women are more likely than men to get very sick.[21] Dengue can be life-threatening in people with chronic (long-lasting) diseases, like diabetes and asthma.[21]
There are four different types of the dengue virus. Once a person has had one type of the virus, he usually is protected from that type for the rest of his life. However, he will only be protected against the other three types of the virus for a short time. If he later gets one of those three types of the virus, he will be more likely to have serious problems, like dengue shock syndrome or dengue hemorrhagic fever.[7][22]
Diagnosis[change | change source]
Usually, doctors diagnose dengue by examining the infected person and realizing that their symptoms match dengue.[2] However, when dengue is in its early stages, it can be difficult to tell the difference between this disease and other infections caused by viruses.[7]
The World Health Organization says that a person probably has dengue if:[8]
- He has a fever; AND
- He has two of these symptoms:
- Nausea and vomiting;
- A rash;
- Pain all over the body;
- A low number of white blood cells; or
- A positive tourniquet test. (To do this test, a doctor wraps a blood pressure cuff around a person's arm for five minutes, then counts any red spots on the skin. If the person has many spots, they are more likely to have dengue fever.)
The World Health Organization also says that in areas where dengue is common, any warning signs, plus a fever, usually signal that a person has dengue fever.[23]
Blood tests[change | change source]
Some blood tests show changes when a person has dengue fever. The earliest change is a low number of white blood cells in the blood. A low number of platelets can also signal dengue.[7] Special blood tests can look for the dengue virus itself; the virus's nucleic acids; or the antibodies that the immune system makes to fight off the virus.[21][24] However, these special tests are expensive.[24] Also, in many areas where dengue is common, most doctors and clinics do not have laboratories for blood tests or special machines.[2]
It can be difficult to tell the difference between dengue fever and chikungunya. Chikungunya is a similar viral infection that has many of the same symptoms of dengue, and happens in the same parts of the world.[11] Dengue can also have some of the same symptoms as other diseases, like malaria, leptospirosis, typhoid fever, and meningococcal disease. Often, before a person is diagnosed with dengue, their doctor will do tests to make sure they do not actually have one of these diseases instead.[7]
WHO classification systems[change | change source]
In 1997, the World Health Organization (WHO) created a system for describing the different types of dengue fever. Eventually, the WHO decided that this old way of dividing dengue needed to be simpler. It also decided that not everyone with dengue fever fit into the old categories. In 2009, the WHO changed its system for classifying (dividing) dengue fever. However, the older system often is still used.[7][23][25]
The old system[change | change source]
The WHO's old system divided dengue into three categories:[23][25]
- Undifferentiated fever
- Dengue fever
- Dengue hemorrhagic fever. This was then divided into four stages, called grades I-IV:
- In Grade I, the person has a fever. He also bruises easily or has a positive tourniquet test.
- In Grade II, the person bleeds into the skin and other parts of the body.
- In Grade III, the person shows signs of circulatory shock. This is called dengue shock syndrome.
- In Grade IV, the person has shock so severe that his blood pressure and heartbeat cannot be felt. This is a more serious version of dengue shock syndrome.[25]
The new system[change | change source]
In 2009, the WHO created a simpler system which divided dengue fever into two types:[2][23]
- Uncomplicated: People who just have the febrile stage of dengue fever, and never go into the critical phase. They get better on their own or just need basic medical help.
- Severe: People who have symptoms that could kill them, or have serious complications from dengue.
Prevention[change | change source]
There are no vaccines that can keep people from getting the dengue virus.[2] The best ways to prevent dengue are to protect people from mosquito bites and to control the mosquito population.[26][26]
The best way to control the mosquito is to get rid of the places it lives. The best way to do this is to get rid of areas with standing water (water that does not move). Mosquitoes like standing water and often lay its eggs there. To prevent getting bitten by mosquitoes, people can:
- Wear clothing that fully covers their skin
- Use bug spray
- Use mosquito netting when they are resting.
Integrated Vector Control[change | change source]
The WHO suggests a program for preventing dengue (called an "Integrated Vector Control" program) that includes five different parts:[26]
- Advocacy, people working together, and legislation (laws) should be used to make public health organizations and communities stronger.
- All parts of society should work together. This includes the public sector (like the government), the private sector (like businesses and corporations), and the health care field.
- All ways of controlling disease should be brought together.
- Decisions should be make based on evidence. This will help make sure that the things that are done to address dengue are helpful.
- Areas where dengue is a problem should be given help, so that they can build their abilities to respond well to the disease on their own.
Treatment[change | change source]

There are no specific treatments for dengue fever.[2] No known anti-viral medications (medicines which kill viruses) will kill the dengue virus. Health workers can give "supportive treatment" - treat dengue's symptoms to try to make patients feel better. Different people need different treatments, depending on their symptoms. Some people can get better just by drinking fluids at home, and checking with their doctor to make sure they are getting better.
Treating dehydration is very important. Sometimes, people are so dehydrated that they need intravenous fluids - fluids given through a needle placed into a vein. Usually, people only need intravenous fluids for a day or two.[27]
Doctors can give medicines like acetaminophen (paracetamol) for fever and pain. Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and aspirin should not be used because they make bleeding more likely.[27]
People with bad dengue may need blood transfusions. Having extra blood will help a person if their blood pressure is getting very low (like it does in dengue shock syndrome) or if they do not have enough red blood cells in their blood (because they are bleeding from dengue hemorrhagic fever).[28]
When people reach the recovery stage of dengue, doctors usually stop giving intravenous fluids to prevent fluid overload (having too much fluid in the body). If a person gets fluid overload, doctors can give a type of medication called a diuretic, which will make the patient urinate out the extra fluid.[28]
Prognosis[change | change source]
Most people with dengue recover and don't have any problems afterward.[23] Without treatment, 1% to 5% of infected people die from dengue.[7] With good treatment, less than 1% die.[23] However, 26% of people with severe dengue die.[7]
Epidemiology[change | change source]
Dengue is common in more than 110 countries.[7] Every year, it infects 50 to 100 million people around the world. It also causes half a million hospitalizations[2] and about 12,500 to 25,000 deaths .[6][29] The World Health Organization says that dengue fever is not taken as seriously as it should be. It calls dengue one of 16 "neglected tropical diseases" - diseases which do not get enough attention.[30] In every million people, dengue causes about 1600 years of life to be lost. This is about the same as other tropical and deadly diseases, like tuberculosis.[21] However, the WHO says the neglected tropical diseases, like dengue, do not get the attention and money that is needed to find treatments and cures.
Dengue is becoming much more common around the world. It is the most common viral disease that is spread by arthropods.[22] In 2010, dengue was 30 times more common than it was in 1960.[31] Scientists think dengue may be getting more common because:
- More people are living in cities.
- There are more people in the world. The world's population is growing.
- More people are travelling internationally (between countries).
- Global warming is thought to play a part in the increase in dengue.[2]
Dengue happens most around the equator. 2.5 billion people live in areas where dengue happens. 70% of these people live in Asia and the Pacific.[31] In the United States, 2.9% to 8% of people who come back from traveling in areas where dengue happens, and have a fever, were infected while traveling.[15] In this group of people, dengue is the second most common infection to be diagnosed, after malaria.[11]
History[change | change source]
Dengue fever is probably a very old disease. An ancient Chinese medical encyclopedia from the Jin Dynasty (which existed from 265 to 420 AD) talked about a person who probably had dengue. The book talked about a "water poison" that had to do with flying insects.[32][33]
Written records from the 17th century talk about what may have been epidemics of dengue (where the disease spread very quickly in a short time). The most likely early reports of dengue epidemics are from 1779 and 1780. These reports talk about an epidemic that spread across Asia, Africa, and North America.[33] From that time until 1940, there were not many more epidemics.[33]
In 1906, scientists proved that people were getting infections from Aedes mosquitoes. In 1907, scientists showed that a virus causes dengue. This was just the second disease that was shown to be caused by a virus. (The first was yellow fever.)[34] John Burton Cleland and Joseph Franklin Siler kept studying the dengue virus, and figured out the basics of how the virus spreads.[34]
Dengue began to spread much more quickly during and after World War II. Different types of dengue also spread to new areas. For the first time, people started to get dengue hemorrhagic fever. The first case of dengue hemorrhagic fever happened in the Philippines in 1953. By the 1970s, dengue hemorrhagic fever had become a major cause of death in children. It also spread to the Pacific and the Americas.[33] Dengue hemorrhagic fever and dengue shock syndrome were first reported in Central America and South America in 1981.
History of the word[change | change source]
It is not clear where the word "dengue" came from. Some people think that it comes from the Swahili phrase Ka-dinga pepo. This phrase talks about the disease being caused by an evil spirit.[32] The Swahili word dinga is thought to come from the Spanish word dengue, which means "careful." That word may have been used to describe a person having bone pain from dengue fever; that pain would make the person walk carefully.[35] However, it is also possible that the Spanish word came from the Swahili word, and not the other way around.[32]
Other people think that the name "dengue" comes from the West Indies. In the West Indies, slaves that had dengue were said to stand and walk like "a dandy." Because of this, the disease was also called "dandy fever."[36][37]
The name "breakbone fever" was first used by Benjamin Rush, a doctor and United States "Founding Father." In 1789, Rush used the name "breakbone fever" in a report about the 1780 dengue outbreak in Philadelphia. In his official report, Rush mostly used the more formal name "bilious remitting fever".[38][39]
The term "dengue fever" was not commonly used until after 1828.[37] Before that, different people used different names for the disease. For example, dengue was also called "breakheart fever" and "la dengue."[37] Other names were also used for severe dengue: for example, "infectious thrombocytopenic purpura", "Philippine," "Thai," and "Singapore hemorrhagic fever."[37]
Research[change | change source]
Scientists keep doing research on ways to prevent and treat dengue. People are also working on controlling mosquitoes,[40] creating a vaccine, and creating drugs to fight the virus.[26]
Many simple things have been done to control mosquitoes. Some of these things have worked. For example, guppies (Poecilia reticulata) or copepods can be put in standing water to eat the mosquito larvae (eggs).[40]
Scientists also keep working on creating antiviral drugs to treat attacks of dengue fever and keep people from getting severe complications.[41][42] They are also working on figuring out how the virus's proteins are structured. This may help them create medications that work well for dengue.[43]
Notes[change | change source]
- ↑ "Brazil warns dengue cases could hit 5mn as extreme weather takes toll". www.ft.com. Retrieved 2024-01-08.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Whitehorn J, Farrar J (2010). "Dengue". Br. Med. Bull. 95: 161–73. doi:10.1093/bmb/ldq019. PMID 20616106.
- ↑ 3.0 3.1 WHO (2009), pp. 14–16.
- ↑ 4.0 4.1 Reiter P (2010-03-11). "Yellow fever and dengue: a threat to Europe?". Euro Surveil. 15 (10): 19509. doi:10.2807/ese.15.10.19509-en. PMID 20403310.
- ↑ Gubler (2010), p. 379.
- ↑ 6.0 6.1 6.2 6.3 Varatharaj A (2010). "Encephalitis in the clinical spectrum of dengue infection". Neurol. India. 58 (4): 585–91. doi:10.4103/0028-3886.68655. PMID 20739797.
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 7.11 7.12 7.13 7.14 7.15 Ranjit S, Kissoon N (July 2010). "Dengue hemorrhagic fever and shock syndromes". Pediatr. Crit. Care Med. 12 (1): 90–100. doi:10.1097/PCC.0b013e3181e911a7. PMID 20639791. S2CID 10135251.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 WHO (2009), pp. 25–27.
- ↑ Kevin J. Knoop (2010). Atlas of emergency medicine (3rd ed.). New York: McGraw-Hill Professional. ISBN 978-0-07-149618-6. OCLC 276338122.
- ↑ 10.0 10.1 10.2 10.3 Gould EA, Solomon T (February 2008). "Pathogenic flaviviruses". The Lancet. 371 (9611): 500–9. doi:10.1016/S0140-6736(08)60238-X. PMID 18262042. S2CID 205949828.
- ↑ 11.0 11.1 11.2 11.3 11.4 Chen LH, Wilson ME (October 2010). "Dengue and chikungunya infections in travelers". Curr. Opin. Infect. Dis. 23 (5): 438–44. doi:10.1097/QCO.0b013e32833c1d16. PMID 20581669. S2CID 2452280.
- ↑ Wolff K; Johnson RA, eds. (2009). "Viral Infections of Skin and Mucosa". Fitzpatrick's Color Atlas and Synopsis of Clinical Dermatology (6th ed.). New York: McGraw-Hill Medical. pp. 810–2. ISBN 9780071599757.
- ↑ Kamel MG, Nam NT, Han NHB, El-Shabouny A-E, Makram A-EM, Abd-Elhay FA-E, | display-authors = etal (2017) Post-dengue acute disseminated encephalomyelitis: A case report and meta-analysis. PLoS Negl Trop Dis 11(6): e0005715. https://doi.org/10.1371/journal.pntd.0005715
- ↑ Gubler (2010), pp. 377–78.
- ↑ 15.0 15.1 Center for Disease Control and Prevention. "Chapter 5 – Dengue Fever (DF) and Dengue Hemorrhagic Fever (DHF)". 2010 Yellow Book. Retrieved 2010-12-23.
- ↑ Wilder-Smith, Annelies; Chen, Lin H.; Massad, Eduardo; Wilson, Mary E. (January 2009). "Threat of Dengue to Blood Safety in Dengue-Endemic Countries". Emerging Infectious Diseases. 15 (1): 8–11. doi:10.3201/eid1501.071097. ISSN 1080-6040. PMC 2660677. PMID 19116042.
- ↑ Stramer, Susan L.; Hollinger, F. Blaine; Katz, Louis M.; Kleinman, Steven; Metzel, Peyton S.; Gregory, Kay R.; Dodd, Roger Y. (August 2009). "Emerging infectious disease agents and their potential threat to transfusion safety". Transfusion. 49: 1S–29S. doi:10.1111/j.1537-2995.2009.02279.x. PMID 19686562. S2CID 24447855.
- ↑ Teo, D.; Ng, L. C.; Lam, S. (April 2009). "Is dengue a threat to the blood supply?". Transfusion Medicine. 19 (2): 66–77. doi:10.1111/j.1365-3148.2009.00916.x. PMC 2713854. PMID 19392949.
- ↑ Wiwanitkit V (January 2010). "Unusual mode of transmission of dengue". Journal of Infection in Developing Countries. 4 (1): 51–4. doi:10.3855/jidc.145. PMID 20130380.
- ↑ Martina, Byron E. E.; Koraka, Penelope; Osterhaus, Albert D. M. E. (October 2009). "Dengue Virus Pathogenesis: an Integrated View". Clinical Microbiology Reviews. 22 (4): 564–581. doi:10.1128/CMR.00035-09. ISSN 0893-8512. PMC 2772360. PMID 19822889.
- ↑ 21.0 21.1 21.2 21.3 Guzman, Maria G.; Halstead, Scott B.; Artsob, Harvey; Buchy, Philippe; Farrar, Jeremy; Gubler, Duane J.; Hunsperger, Elizabeth; Kroeger, Axel; Margolis, Harold S.; Martínez, Eric; Nathan, Michael B. (December 2010). "Dengue: a continuing global threat". Nature Reviews Microbiology. 8 (S12): S7–S16. doi:10.1038/nrmicro2460. ISSN 1740-1526. PMC 4333201. PMID 21079655.
- ↑ 22.0 22.1 Rodenhuis-Zybert, Izabela A.; Wilschut, Jan; Smit, Jolanda M. (August 2010). "Dengue virus life cycle: viral and host factors modulating infectivity". Cellular and Molecular Life Sciences. 67 (16): 2773–2786. doi:10.1007/s00018-010-0357-z. ISSN 1420-682X. PMID 20372965. S2CID 4232236.
- ↑ 23.0 23.1 23.2 23.3 23.4 23.5 WHO (2009), pp. 10–11.
- ↑ 24.0 24.1 WHO (2009), pp. 90–95.
- ↑ 25.0 25.1 25.2 WHO (1997). "Chapter 2: clinical diagnosis". Dengue haemorrhagic fever: diagnosis, treatment, prevention and control (PDF) (2nd ed.). Geneva: World Health Organization. pp. 12–23. ISBN 9241545003.
- ↑ 26.0 26.1 26.2 26.3 WHO (2009), pp. 59–60.
- ↑ 27.0 27.1 WHO (2009), pp. 32–37.
- ↑ 28.0 28.1 WHO (2009), pp. 40–43.
- ↑ WHO media centre (March 2009). "Dengue and dengue haemorrhagic fever". World Health Organization. Retrieved 2010-12-27.
- ↑ Neglected Tropical Diseases. "Diseases covered by NTD Department". World Health Organization. Retrieved 2010-12-27.
- ↑ 31.0 31.1 WHO (2009), p. 3.
- ↑ 32.0 32.1 32.2 Anonymous (2006). "Etymologia: dengue" (PDF). Emerg. Infec. Dis. 12 (6): 893. doi:10.3201/eid1206.ET1206. S2CID 29398958.
- ↑ 33.0 33.1 33.2 33.3 Gubler DJ (July 1998). "Dengue and Dengue Hemorrhagic Fever". Clin. Microbiol. Rev. 11 (3): 480–96. doi:10.1128/CMR.11.3.480. PMC 88892. PMID 9665979. Archived from the original on 2011-10-25. Retrieved 2012-02-10.
- ↑ 34.0 34.1 Henchal EA, Putnak JR (October 1990). "The dengue viruses". Clin. Microbiol. Rev. 3 (4): 376–96. doi:10.1128/CMR.3.4.376. PMC 358169. PMID 2224837. Archived from the original on 2011-07-25. Retrieved 2012-02-10.
- ↑ Harper D (2001). "Etymology: dengue". Online Etymology Dictionary. Retrieved 2008-10-05.
- ↑ Anonymous (1998-06-15). "Definition of Dandy fever". MedicineNet.com. Archived from the original on 2011-06-05. Retrieved 2010-12-25.
- ↑ 37.0 37.1 37.2 37.3 Halstead SB (2008). Dengue (Tropical Medicine: Science and Practice). River Edge, N.J: Imperial College Press. pp. 1–10. ISBN 978-1-84816-228-0.
- ↑ Barrett AD, Stanberry LR (2009). Vaccines for biodefense and emerging and neglected diseases. San Diego: Academic. pp. 287–323. ISBN 978-0-12-369408-9.
- ↑ Rush AB (1789). "An account of the bilious remitting fever, as it appeared in Philadelphia in the summer and autumn of the year 1780". Medical enquiries and observations. Philadelphia: Prichard and Hall. pp. 104–117.
- ↑ 40.0 40.1 WHO (2009), p. 71.
- ↑ Sampath A, Padmanabhan R (January 2009). "Molecular targets for flavivirus drug discovery". Antiviral Res. 81 (1): 6–15. doi:10.1016/j.antiviral.2008.08.004. PMC 2647018. PMID 18796313.
- ↑ Noble, Christian G.; Chen, Yen-Liang; Dong, Hongping; et al. (March 2010). "Strategies for development of dengue virus inhibitors". Antiviral Research. 85 (3): 450–462. doi:10.1016/j.antiviral.2009.12.011. PMID 20060421.
- ↑ Noble, Christian G.; Chen, Yen-Liang; Dong, Hongping; Gu, Feng; Lim, Siew Pheng; Schul, Wouter; Wang, Qing-Yin; Shi, Pei-Yong (March 2010). "Strategies for development of dengue virus inhibitors". Antiviral Research. 85 (3): 450–462. doi:10.1016/j.antiviral.2009.12.011. PMID 20060421.
References[change | change source]
- Gubler DJ (2010). "Dengue viruses". In Mahy BWJ, Van Regenmortel MHV (ed.). Desk Encyclopedia of Human and Medical Virology. Boston: Academic Press. pp. 372–82. ISBN 978-0-12-375147-8.
- WHO (2009). Dengue Guidelines for Diagnosis, Treatment, Prevention and Control (PDF). Geneva: World Health Organization. ISBN 978-9241547871.
